Meniscus tears are one of the most common knee injuries among active adults. Whether caused by a twisting movement on the trail, years of repetitive loading, or gradual degeneration, a torn meniscus can lead to persistent pain, swelling, and reduced performance.
Traditionally, treatment options were limited to rest, physical therapy, cortisone injections, or arthroscopic surgery. But regenerative medicine has changed the conversation. Today, stem cell therapy for knees offers a non-surgical option—especially when chosen carefully based on tear type.
At Dynamic Athlete, we evaluate whether MFAT (Microfragmented Adipose Tissue) or BMA (Bone Marrow Aspirate) is more appropriate depending on the structure and severity of the tear.
Understanding the difference is essential before searching for stem cell therapy near me.
Why Meniscus Tears Don’t Always Heal on Their Own
The meniscus has limited blood supply—especially in its inner zones. Tears located in poorly vascularized regions struggle to heal without intervention.
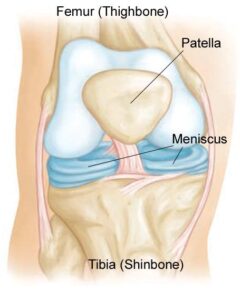
Common meniscus tear types include:
- Radial tears
- Horizontal cleavage tears
- Complex degenerative tears
- Root tears
- Flap tears
Each type responds differently to regenerative treatment.
This is why selecting the correct biologic source matters.
Stem Cell Therapy for Knees: How It Works
Stem cell therapy for knees uses your body’s own regenerative cells to support tissue healing, reduce inflammation, and improve joint environment.
Two primary biologic sources are used:
1. MFAT (Microfragmented Adipose Tissue)
Derived from fat tissue, MFAT contains:
- Mesenchymal stem cells
- Growth factors
- Anti-inflammatory cytokines
MFAT is often beneficial for:
- Degenerative meniscus tears
- Chronic joint inflammation
- Early to moderate arthritis
Because it has strong anti-inflammatory properties, MFAT may be ideal when meniscus damage overlaps with stem cell therapy for knee arthritis scenarios.
2. BMA (Bone Marrow Aspirate)
Harvested from bone marrow, BMA contains:
- Stem cells
- Platelets
- Growth factors
- Progenitor cells
BMA may be more appropriate for:
- Traumatic tears
- Tears with healing potential
- Younger patients with better tissue quality
BMA is often selected when the goal is stronger regenerative stimulation rather than primarily inflammation control.
MFAT vs BMA: Choosing Based on Tear Type
Degenerative Tears
Common in runners and active adults over 40, degenerative tears often coexist with cartilage wear.
In these cases:
- MFAT may provide better anti-inflammatory modulation
- Joint environment improvement is prioritized
- Combined rehab enhances outcomes
Traumatic Tears
Acute twisting injuries with clearer tear margins may benefit more from BMA’s stronger regenerative signaling.
The decision depends on:
- MRI findings
- Tear location
- Tissue viability
- Activity goals
At Dynamic Athlete, imaging and functional evaluation guide the biologic choice.
Stem Cell Therapy Cost: What Affects Pricing?
Patients often search for stem cell therapy cost before understanding what determines value.
Pricing depends on:
- Type of biologic (MFAT vs BMA)
- Imaging guidance
- Preparation technique
- Clinical expertise
- Rehab integration
Lower-cost clinics may not tailor treatment to tear type. When evaluating a stem cell clinic near me, expertise matters more than proximity.
Can Stem Cell Therapy Replace Surgery?
Not all meniscus tears require surgery. Many partial tears and degenerative tears can be managed with regenerative therapy and proper load management.
Stem cell therapy aims to:
- Preserve native tissue
- Improve joint environment
- Reduce pain
- Restore activity tolerance
However, full-thickness displaced tears or mechanical locking symptoms may still require surgical consultation.
Honest patient selection is critical.
What About Other Joint Injuries?
Regenerative therapies extend beyond the knee.
For example:
- Stem cell therapy for rotator cuff tear may be used for partial tendon tears in the shoulder.
- Stem cell therapy for knee arthritis focuses on preserving cartilage and reducing inflammation.
The key principle remains the same: choose the biologic based on tissue type and injury characteristics.
Who Is a Good Candidate for Stem Cell Therapy for Knees?
Ideal candidates:
- Have partial meniscus tears
- Experience chronic knee pain
- Want to avoid surgery
- Have mild to moderate arthritis
- Are committed to structured rehab
Stem cell therapy is not a quick fix. It requires:
- Proper diagnosis
- Precise injection technique
- Controlled reloading
- Strength progression
Why Dynamic Athlete Takes a Customized Approach
At Dynamic Athlete, we don’t treat every meniscus tear the same.
Our process includes:
- Detailed movement assessment
- Imaging review
- Tear-type classification
- Biologic selection (MFAT or BMA)
- Structured return-to-activity planning
We view regenerative medicine as part of a system—not a standalone injection.
Stem Cell Therapy Near Me: What to Ask Before Choosing
Before selecting a provider, ask:
- How do you determine MFAT vs BMA?
- Is imaging guidance used?
- Is rehab integrated?
- What are realistic timelines?
The right questions protect both your knee and your investment.
Final Thoughts
Meniscus tears are not all the same—and neither are regenerative treatments.
Choosing between MFAT and BMA should depend on tear type, tissue quality, and long-term goals. When applied correctly, stem cell therapy for knees offers a joint-preserving alternative to surgery—especially for active adults who want to stay active.
If you’re considering stem cell therapy near me, make sure the plan is tailored—not generic.
At Dynamic Athlete, our goal is simple: preserve your joint, restore your performance, and help you move forward with confidence.







